Higher Blood Pressure Ties to Heart and Kidney Disease: What You Need Now
Higher Blood Pressure Ties to Heart and Kidney Disease: What You Need Now
Even a modest rise in blood pressure can push heart and kidney disease risk higher, and that is the mainKeyword on every clinician’s mind right now. You feel fine, the cuff reads 125/78, and you assume you are safe. But studies now show damage can start below the old thresholds, especially in midlife. The stakes are real: clogged arteries, stiff hearts, and kidneys that lose filtering power. You need clear numbers, practical steps, and fast ways to course-correct without panic.
Why This Shift Matters Today
- New research links higher blood pressure to earlier heart and kidney strain.
- Risk rises even in the upper end of “normal” readings.
- Home monitoring can spot patterns your annual checkup misses.
- Small lifestyle changes can shave points off your readings quickly.
Reading the Numbers on High Blood Pressure Risk
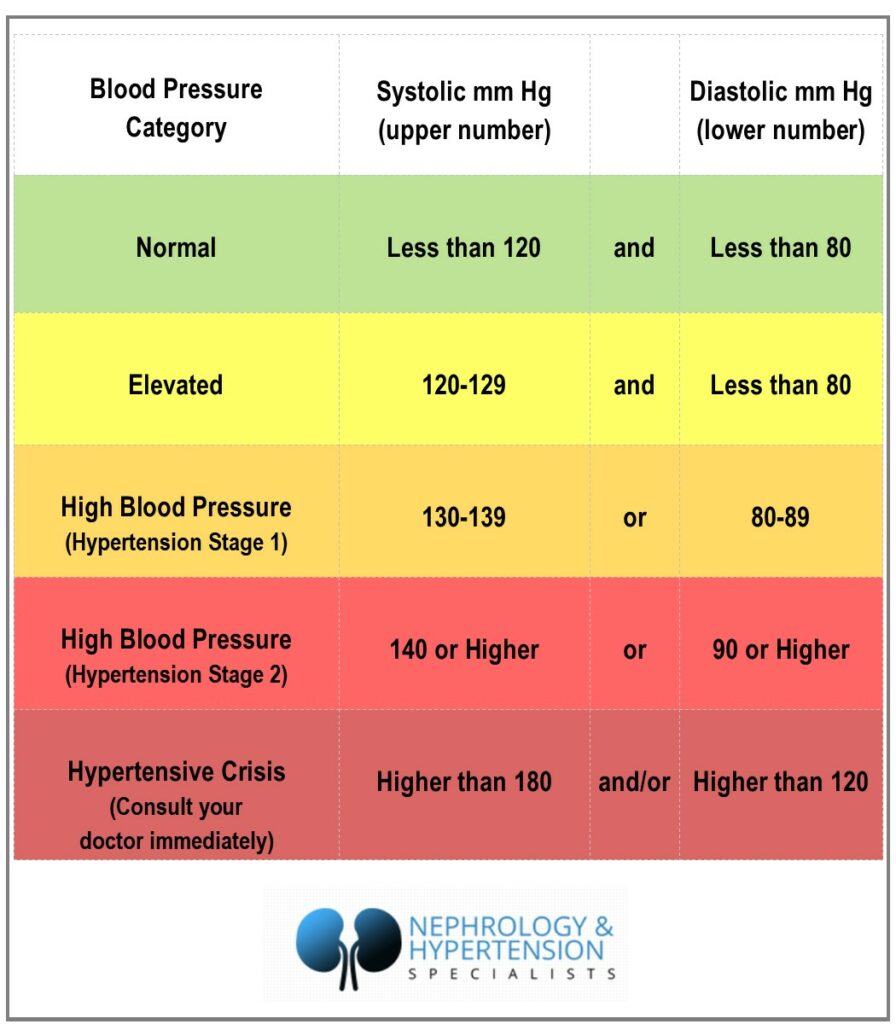
Your systolic number creeping toward 130 is not a shrug; it is a warning light. The study highlighted that higher blood pressure harms kidney vessels over time, and that damage often appears before symptoms. Think of your arteries like plumbing in an old house: a little extra pressure speeds up leaks. Do you want to wait for the ceiling to sag?
“Lower targets pay off for the heart and kidneys,” said one researcher who reviewed the findings.
One-sentence truth: Consistent readings above 120/80 deserve action.
How to Act Fast on the mainKeyword
- Track at home twice a day for two weeks. Record morning and evening readings to catch spikes.
- Cut sodium to under 1,500 mg daily. Swap canned soups and deli meats for fresh options.
- Add 20 to 30 minutes of brisk walking most days. Treat it like a daily appointment.
- Limit alcohol to no more than one drink a day. Alcohol can nudge numbers upward.
- Discuss medication if averages stay high. Low-dose thiazides or ACE inhibitors are common first steps.
Monitoring Heart and Kidney Signals
Ask for a basic metabolic panel to check creatinine and eGFR alongside your blood pressure log. That pairing shows whether kidneys are already straining. And a simple ECG can catch early heart changes. Look, you would not drive a car with a blinking oil light and skip the mechanic; your organs deserve the same respect.
Home Tech That Helps
Choose a validated upper arm cuff, not a wrist gadget. Sync results to a health app so you and your clinician see trends. But do not chase every blip; focus on weekly averages.
Cutting Risk Through Daily Habits
Think of meal prep like setting a basketball pick: it sets up an easy shot later. Batch-cook beans, roast vegetables, and keep low-sodium spice blends handy. Swap saturated fats for olive oil. Sleep seven to eight hours to keep cortisol and pressure in check. If stress drives spikes, try five-minute breathing drills between meetings.
When to Call Your Clinician
Call within a week if home averages stay above 130/80. Seek urgent care if you see 180/120 with chest pain, shortness of breath, or vision changes. Share your full log; context helps avoid overtreatment.
What This Means for Your Next Decade
Acting on the mainKeyword now keeps arteries flexible and kidneys filtering well into your 50s and beyond. I have covered blood pressure guidelines for two decades, and the through-line is simple: early action beats late rescue. Will you wait for symptoms, or bank healthier years starting this week?
Sources
This article was medically reviewed and draws from peer-reviewed research and clinical guidelines published by:
- National Institute on Drug Abuse (NIDA)
- Substance Abuse and Mental Health Services Administration (SAMHSA)
- Centers for Disease Control and Prevention (CDC)
- MedlinePlus — U.S. National Library of Medicine
Content is reviewed for medical accuracy by our editorial team. Last reviewed: April 5, 2026.
Medical Disclaimer: This article is for educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider before making changes to your treatment plan. If you are experiencing a medical emergency, call 911 immediately. For substance use support, call SAMHSA at 1-800-662-4357 (free, confidential, 24/7).