Gabapentin: Uses, Risks, and Potential for Abuse
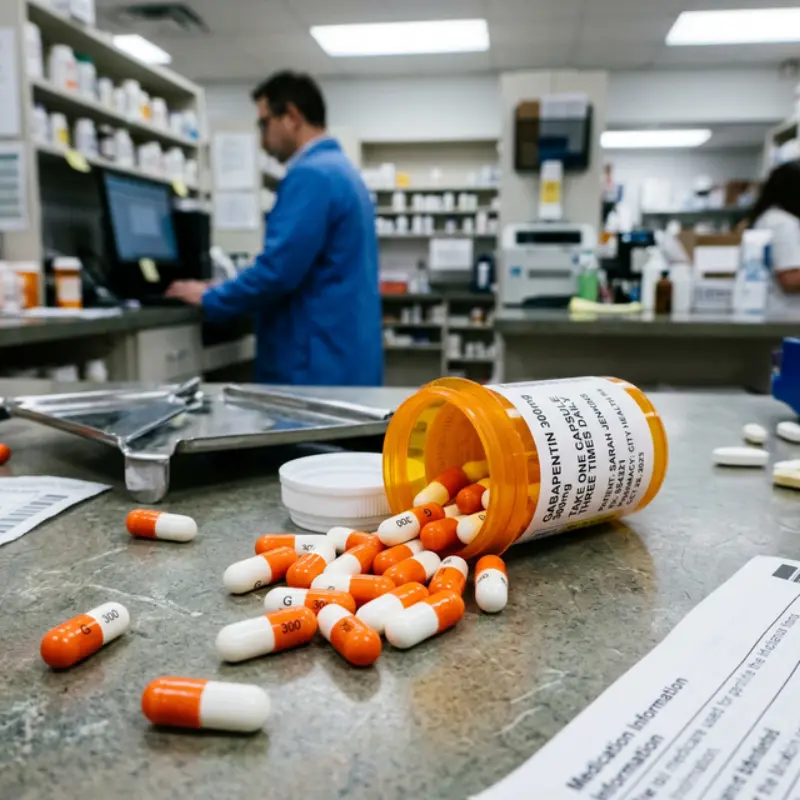
What is Gabapentin?
Gabapentin (brand name Neurontin) is a prescription medication originally developed to treat epileptic seizures. Doctors now prescribe gabapentin for nerve pain, restless leg syndrome, and as an off-label treatment for anxiety and alcohol withdrawal. Despite its widespread use, gabapentin carries a growing risk of misuse and dependence. Several states have reclassified gabapentin as a controlled substance in response to rising abuse rates.
If you or someone you know takes gabapentin, understanding the risks of misuse, the signs of dependence, and your treatment options protects against a problem many people do not see coming.
What You Should Know About Gabapentin
- Gabapentin is not federally classified as a controlled substance, but at least 7 states now classify gabapentin as Schedule V
- Gabapentin prescriptions exceeded 69 million in 2019, making gabapentin one of the most prescribed medications in the U.S.
- Studies show gabapentin is present in roughly 1 in 3 opioid overdose deaths
- Misuse rates are highest among people with a history of opioid or alcohol use disorders
How Gabapentin Works
Gabapentin acts on your nervous system by modifying the activity of GABA, a neurotransmitter responsible for calming nerve signals. The medication reduces abnormal electrical activity in the brain (preventing seizures) and blocks pain signals traveling through damaged nerves.
At prescribed doses, gabapentin does not produce a high. At elevated doses, especially when combined with opioids or alcohol, gabapentin creates feelings of relaxation, euphoria, and sedation similar to benzodiazepines.
Approved Medical Uses
- Epilepsy: gabapentin prevents partial seizures when used alongside other anti-seizure medications
- Postherpetic neuralgia: the drug treats nerve pain following shingles outbreaks
- Restless leg syndrome: gabapentin enacarbil (Horizant) is FDA-approved for this condition
Common Off-label Uses
- Diabetic neuropathy (nerve pain from diabetes)
- Fibromyalgia pain management
- Anxiety disorders
- Alcohol withdrawal management
- Hot flashes during menopause
Why Gabapentin Misuse Is Increasing
Gabapentin misuse has risen sharply since 2015 for several reasons:
- Availability: gabapentin is prescribed more freely than opioids or benzodiazepines because many providers still view gabapentin as low-risk
- Opioid enhancement: people using opioids take gabapentin to intensify the opioid high. This combination dramatically increases overdose risk.
- Opioid substitution: when opioid prescriptions are restricted, some patients turn to gabapentin as an alternative
- Difficulty of detection: standard drug screens do not test for gabapentin, making misuse harder to identify
"Gabapentin's emerging role in the overdose crisis demands greater clinical vigilance. Prescribers must weigh the benefits against a real and growing risk of misuse." - Journal of the American Medical Association, 2020
Signs of Gabapentin Misuse
Recognizing gabapentin misuse is difficult because the drug is a legal prescription medication. Watch for these patterns:
- Taking higher doses than prescribed to achieve sedation or euphoria
- Requesting early refills or reporting "lost" prescriptions repeatedly
- Combining gabapentin with opioids, alcohol, or benzodiazepines
- Obtaining gabapentin from multiple doctors or buying from others
- Escalating doses over time without medical guidance
- Withdrawal symptoms (anxiety, insomnia, sweating) when doses are missed
Gabapentin Withdrawal
Physical dependence on gabapentin develops with regular use, especially at high doses. Stopping abruptly is dangerous and causes serious withdrawal symptoms.
Withdrawal Symptoms
- Anxiety and agitation
- Insomnia and sleep disturbances
- Nausea and sweating
- Pain and body aches
- Rapid heart rate
- Seizures (the most dangerous withdrawal complication)
Withdrawal Timeline
- Days 1 to 2: anxiety, insomnia, and nausea begin
- Days 3 to 5: symptoms peak. Seizure risk is highest during this period.
- Days 6 to 14: gradual improvement with lingering anxiety and sleep problems
Never stop gabapentin suddenly. A medical professional creates a tapering schedule, reducing your dose gradually over weeks to minimize withdrawal risk.
Health Risks of Gabapentin Misuse
Overdose Risk
Gabapentin alone rarely causes fatal overdose. The danger multiplies when gabapentin is combined with other central nervous system depressants:
- Gabapentin + opioids: respiratory depression risk increases significantly. The FDA issued a safety warning about this combination in 2019.
- Gabapentin + alcohol: extreme sedation, impaired breathing, and loss of consciousness
- Gabapentin + benzodiazepines: compounding sedation effects leading to respiratory failure
Overdose Signs
- Extreme drowsiness or inability to wake
- Slurred speech and loss of coordination
- Slowed or labored breathing
- Double vision or blurred vision
- Diarrhea
Treatment for Gabapentin Dependence
Recovery from gabapentin dependence requires medical supervision and a structured treatment plan.
Medical Tapering
Your doctor reduces your gabapentin dose by 10% to 25% per week, adjusting the pace based on your symptom response. Tapering schedules typically last 2 to 6 weeks.
Addressing Co-occurring Substance Use
Because gabapentin misuse frequently occurs alongside opioid or alcohol use disorders, effective treatment addresses all substances simultaneously. Integrated treatment programs evaluate and treat the full scope of your substance use.
Therapy and Support
- Cognitive-behavioral therapy (CBT) helps you develop healthier coping strategies for pain, anxiety, or other conditions gabapentin was masking
- Support groups connect you with others who understand the challenges of prescription drug dependence
- Pain management alternatives including physical therapy, nerve blocks, and non-addictive medications replace gabapentin's role in your treatment
Protecting Yourself and Others
If your doctor prescribes gabapentin, take the medication exactly as directed. Report any feelings of euphoria or desire to increase your dose to your prescriber. Store gabapentin securely and never share your medication.
If you recognize signs of gabapentin misuse in yourself or someone around you, professional help is available. Call SAMHSA's National Helpline at 1-800-662-4357 for free, confidential referrals to treatment programs near you.
Sources
This article was medically reviewed and draws from peer-reviewed research and clinical guidelines published by:
- National Institute on Drug Abuse (NIDA)
- Substance Abuse and Mental Health Services Administration (SAMHSA)
- Centers for Disease Control and Prevention (CDC)
- MedlinePlus — U.S. National Library of Medicine
Content is reviewed for medical accuracy by our editorial team. Last reviewed: August 25, 2025.
Medical Disclaimer: This article is for educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider before making changes to your treatment plan. If you are experiencing a medical emergency, call 911 immediately. For substance use support, call SAMHSA at 1-800-662-4357 (free, confidential, 24/7).